06:55
When the world first heard about COVID-19, the initial idea was that it was a respiratory disease, but in recent months experts have realised it can cause serious neurological problems in many patients.
More than 300 studies from around the world have found a prevalence of neurological abnormalities in COVID-19 patients, ranging from delirium, confusion and anxiety to brain inflammation, nerve damage and stroke.
Estimates vary but it seems that around 50 percent of patients diagnosed with COVID-19 have experienced neurological problems. At the mild end of the scale, patients may experience lingering symptoms such as poor memory and tiredness.
But the severe symptoms can result in disability and even death, with growing evidence showing that the virus can, in rare cases, enter the central nervous system.
Acute onset of delirium or encephalopathy is affecting anywhere between 40-50 percent of patients with moderate and severe COVID-19 in hospitals
- Robert Stevens, professor of intensive care at Johns Hopkins Medicine
Robert Stevens, the director of critical care at Johns Hopkins Medicine in the U.S., says the world could be facing a secondary pandemic of neurological disease.
He said: "I'm speaking about these repercussions of infection with the disease and some of which I believe could have, and many of my colleagues believe, could have some long-lasting effects way beyond the acute phase of infection."
Stevens revealed that the neurological complications are wide-ranging: "If we're talking about acute onset of delirium or encephalopathy, this is affecting anywhere between 40-50 percent of patients with moderate and severe COVID-19 in hospitals. This is being shown in a number of different studies.
"And (if) we're talking about stroke, ischemic stroke, this is being documented in three to five percent of people who are hospitalized with COVID-19. If we’re talking about infection of the brain and encephalitis, this is much rarer. As for the other manifestations, things like peripheral nerve disorders and spinal cord inflammation, myelitis, we think that these are quite rare."
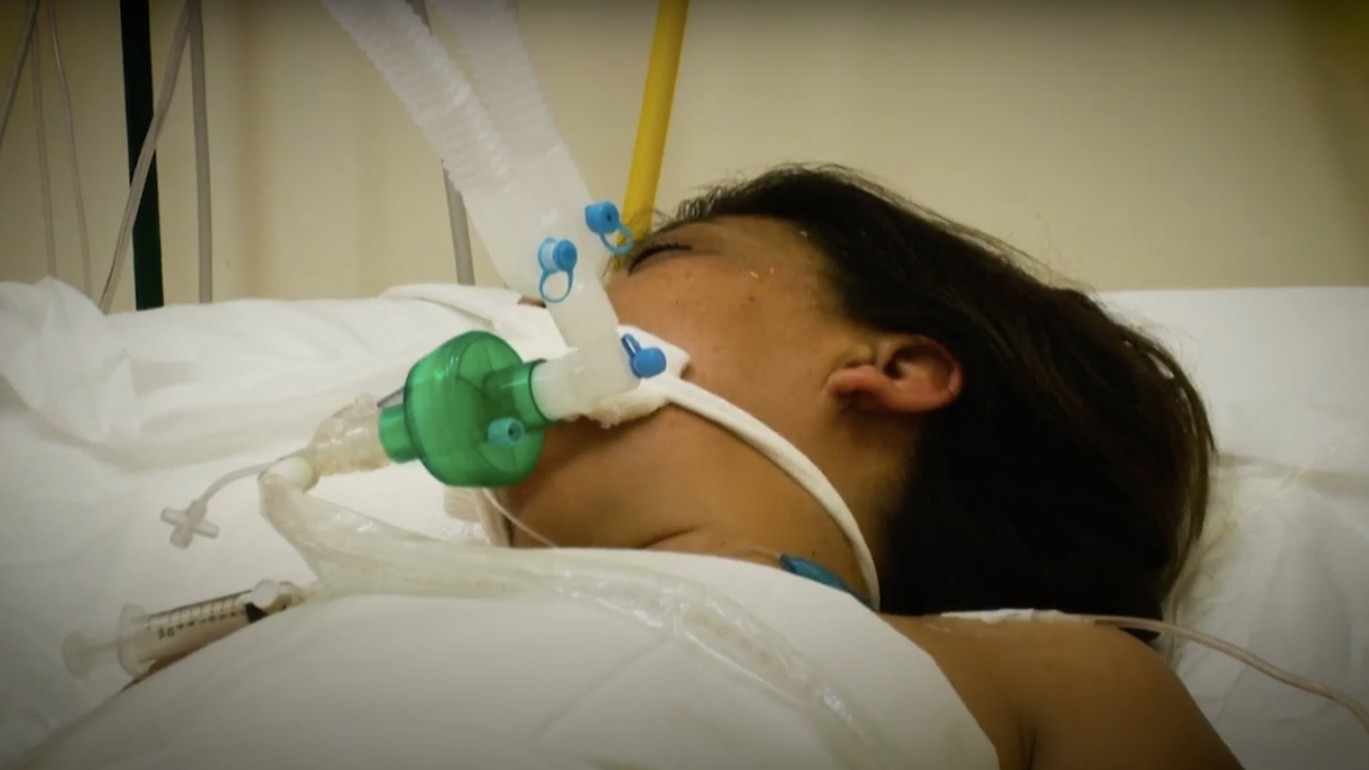
Experts believe that neurological symptoms may have been missed in patients who were put under heavy sedation in hospital. /CGTN
Experts believe that neurological symptoms may have been missed in patients who were put under heavy sedation in hospital. /CGTN
David Strain, from University of Exeter Medical School, has dealt with a number of older adults suffering from neurological issues and says they often suffer from disorientation.
"One of the key features among these individuals was an acute delirium," he explained. "That is, they lost their awareness of their surroundings. They became acutely confused, more so than usual, even in the absence of dementia. And that was far more than we see from similar viral infections."
Doctors believe that the physiological changes in the body and the response of the immune system as it tries to fight the virus are just two of the reasons why patients with moderate and severe symptoms are suffering from brain issues.
Read more: Can ultra-violet light fight COVID-19?
Stevens added: "Their blood oxygen levels can go way down, they can experience very high temperatures, they may experience fluctuations in their blood pressure. And so we believe that those non-specific physiologic alterations can probably affect brain function and may account for a significant proportion of the cases of encephalopathy and delirium.
"The second mechanism we think could be due to the immunological response to the virus. The third mechanism is the hypercoagulable state: we know that many patients, a very, very significant proportion of patients with COVID-19, have a tendency to form blood clots in their veins and arteries. The fourth mechanism is the direct invasion of the brain."
Experts are now calling for clinicians to carry out a thorough neurological examination of COVID-19 patients in order to gain a better understanding of how and why the virus impacts the brain and to limit the long term damage it could cause.
"(It can be that you) can overlook a severe neurological problem in a sedated patient," said Stevens. "And that's why I think we have to have a very high index of suspicion. The physicians taking care of COVID-19 patients should be instructed to perform a very detailed and careful neurological history and examination and immediately either seek consultation with neurologists or obtain additional testing, such as imaging wherever there is a concern about a severe neurological problem."
Read more: World's first COVID-19 lung transplant patient discharged in China